Introduction: Beyond the BMI Number – Unveiling the Full Story of Your Health
You’ve probably heard of BMI, or Body Mass Index. Perhaps you’ve even used one of our General BMI Calculator tools to get your number. It’s a simple calculation, and you might have received a classification: ‘healthy weight,’ ‘overweight,’ or ‘obese.’ But what does that single number truly reveal about your health, and can we trust its BMI accuracy? Many often hold misconceptions about what BMI actually means, leading to questions about its true value. Is it the whole picture, or just the beginning of a much deeper, more personal narrative about your well-being?
For decades, the Body Mass Index has served as a widely recognized and simple screening tool in public health, first introduced by Adolphe Quetelet in the 19th century (Adolphe Quetelet – Wikipedia | Accessed: June 2025). It’s convenient, easy to calculate, and offers a broad overview of weight categories relative to height. Yet, its simplicity often comes with a significant trade-off: nuance. Many people find themselves confused, frustrated, or even misinformed by their BMI result, leading to questions about its accuracy and its real-world implications for their health.
This comprehensive guide will go beyond the simple number. We’re here to demystify BMI, exploring its genuine accuracy, potential risks, and the common myths that often cloud its true meaning. Our goal is to empower you with a more holistic, evidence-based understanding of what your body’s numbers truly mean for your well-being. At BMI Count, we are committed to providing you with truly trustworthy health information, backed by scientific consensus and expert insights, so you can make informed decisions on your health journey.
“Your BMI is a starting point, not the destination. True health is a far richer, more nuanced story.”
BMI Fundamentals: What It Is and How It’s Used (A Quick Primer)
Before we dive into the insights, BMI risks, and BMI misconceptions, let’s quickly recap the basics of what BMI is and its intended purpose.
The Body Mass Index (BMI) is a simple numerical value calculated from a person’s weight and height. It serves as a general indicator of whether a person has a healthy body weight for their height. The formula typically involves dividing a person’s weight in kilograms by the square of their height in meters (
textBMI=
textweight(kg)/
textheight(m)2).
For a complete breakdown of what BMI is, its categories, and how to interpret your results, we encourage you to read our foundational pillar post: Your Complete Guide to Understanding BMI.
Historically, BMI was developed in the 19th century by Adolphe Quetelet, a Belgian astronomer and statistician. His original intent was not to assess individual health or body fat directly, but rather to create a simple metric to track the general weight status of populations. This ease of calculation and application to large datasets is precisely why BMI remains widely used today by public health officials and medical professionals as a preliminary screening tool, despite its well-known limitations of BMI for individuals. It’s cost-effective, non-invasive, and provides a quick estimate that can help identify potential weight-related health issues at a broad, community level, guiding further assessment if needed. The World Health Organization (WHO), for instance, utilizes BMI categories extensively for population-level health surveillance (WHO – Body Mass Index (BMI) | Accessed: June 2025).
The standard BMI categories, as defined by organizations like the WHO and the Centers for Disease Control and Prevention (CDC) (CDC – About Adult BMI | Accessed: June 2025), typically include:
- Underweight: BMI less than 18.5
- Healthy Weight: BMI 18.5 to 24.9
- Overweight: BMI 25.0 to 29.9
- Obesity: BMI 30.0 or higher (often subdivided into Class 1, 2, and 3)
It’s important to remember that these categories are broad guidelines for screening, which is a key concept we’ll explore further as we delve into the nuances of BMI.
“BMI was designed for populations, not precision. It’s a screening tool, not a full health diagnosis.”
Decoding BMI’s “Accuracy”: Strengths and Significant Limitations
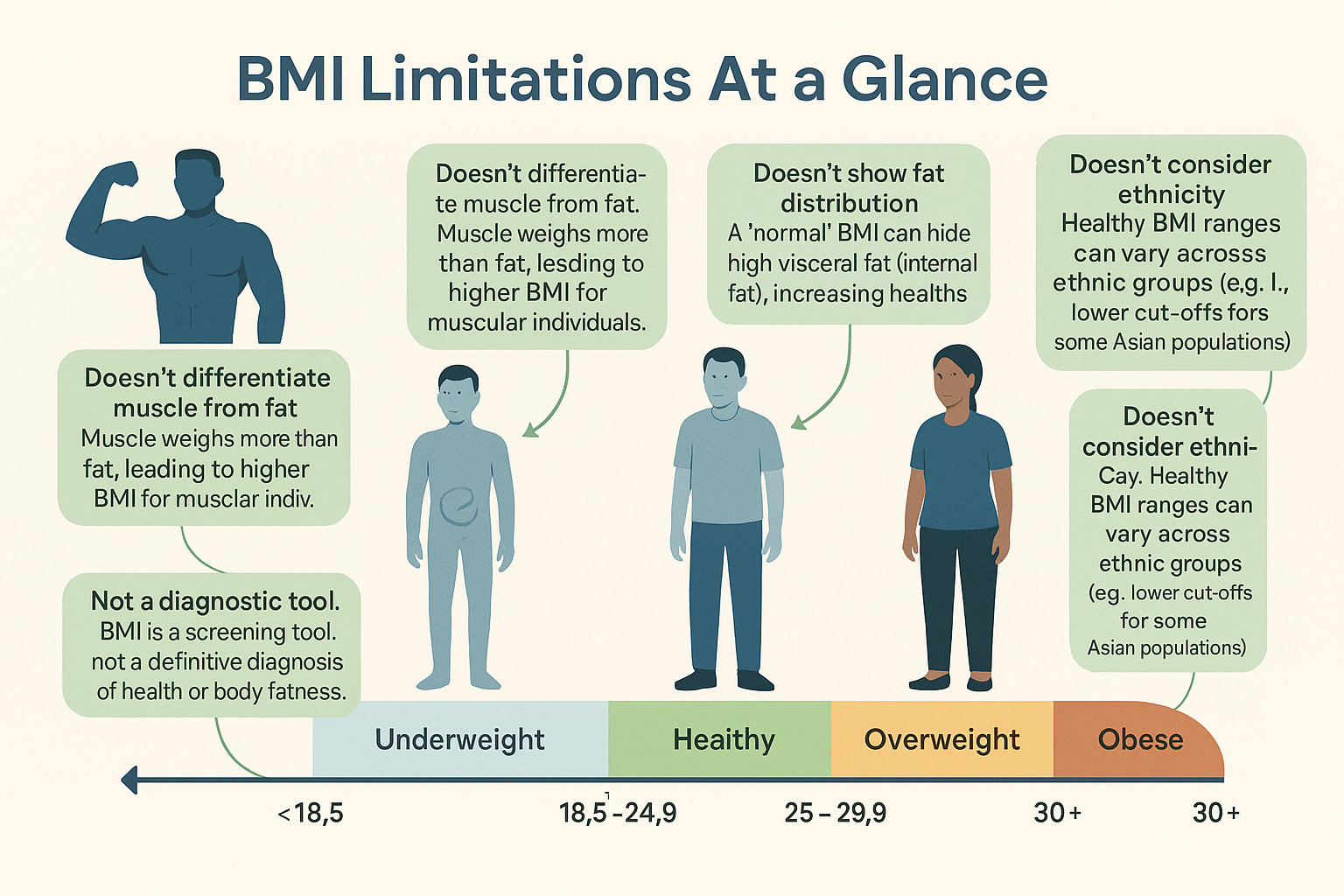
While BMI serves a valuable purpose as a preliminary screening tool, its “BMI accuracy” when applied to individual health assessment is often misunderstood. It’s critical to comprehend where BMI excels and, more importantly, where its inherent limitations of BMI truly become apparent. Understanding these problems with BMI is essential for a holistic view of health, moving beyond BMI as a sole indicator.
Where BMI Shines: Population-Level Insights
At a broad, public health level, BMI is undeniably useful:
- Epidemiological Research: It allows researchers to track obesity trends across large populations over time, helping to inform public health policies and interventions. Organizations like the CDC rely on BMI data to monitor population health status and identify regions requiring public health attention, contributing to an understanding of population-level BMI risks.
- Cost-Effectiveness and Simplicity: It’s an inexpensive and non-invasive metric that can be easily collected from large groups, making it practical for large-scale health surveys and initial screenings. This simplicity is a major reason why it’s widely adopted globally.
- Correlation with Health Risks: Studies involving vast populations consistently show a correlation between higher BMI categories and increased risks for certain chronic diseases like type 2 diabetes, heart disease, stroke, and some cancers. This correlation is why it remains a recognized screening tool to identify individuals who may be at an elevated risk.
Where BMI Falls Short: The Individual Story
The challenges with BMI arise when we try to apply its population-level correlations to individual health assessments. Its fundamental limitations of BMI mean it doesn’t always tell the whole story for a single person:
- It Does Not Differentiate Between Muscle and Fat: This is arguably BMI’s biggest and most frequently cited critique, directly impacting BMI accuracy. BMI simply uses total body weight relative to height, without distinguishing between lean muscle mass and fat mass.
- The Muscular Athlete Paradox: A highly muscular individual, such such as a bodybuilder, weightlifter, or an elite athlete, may have very little body fat but significantly higher muscle mass. Because muscle is denser and weighs more than fat, their BMI could place them in the “overweight” or even “obese” category, despite being in peak physical condition with excellent metabolic health. This misclassification can be frustrating and misleading for athletes and very active individuals. For example, professional football players often have BMIs well over 25 or 30, but possess low body fat percentages
- Actionable Insight & Tool Integration: This is where understanding your unique body composition becomes vital. While BMI provides a starting point, tools that offer deeper insights are crucial. To get a more tailored assessment that indirectly accounts for typical body composition differences, our BMI for Men Calculator and BMI for Women Calculator provide additional metrics such as Ideal Weight Range and Body Surface Area (BSA), helping you get a more nuanced picture beyond the simple weight-to-height ratio.
- It Doesn’t Account for Body Fat Distribution: Where fat is stored on your body significantly impacts health risk, but BMI provides no information on this crucial aspect.
- “Apple” vs. “Pear” Shapes: Individuals who carry more fat around their abdomen (often referred to as an “apple shape,” indicative of higher visceral fat, which surrounds vital organs) generally face higher health risks for conditions like heart disease, type 2 diabetes, and certain cancers, even if their BMI is in the “healthy” range. This is in contrast to those who predominantly carry fat on their hips and thighs (“pear shape,” which is typically subcutaneous fat). Research consistently links higher visceral fat to increased metabolic syndrome risk. BMI cannot differentiate between these fat distributions, making it an incomplete measure for individual risk assessment.
- Future Content Hint: Future discussions will delve into the importance of measures like waist circumference and waist-to-hip ratio, which directly assess abdominal fat and offer critical insights that BMI often misses.
- It Ignores Bone Density and Frame Size: While less impactful than the muscle vs. fat distinction, variations in bone density and overall body frame size can also influence BMI, though typically to a lesser degree. A person with a naturally larger skeletal frame might have a slightly higher BMI without necessarily having excess body fat.
- The “Metabolically Healthy Obese” and “TOFI” (Thin Outside, Fat Inside) Phenomenon: This highlights why simply relying on BMI can be misleading. A “healthy” BMI doesn’t automatically equate to good health, and an “elevated” BMI doesn’t always mean poor health.
- “Metabolically Healthy Obese” (MHO): Some individuals who fall into the “overweight” or “obese” BMI categories may exhibit healthy metabolic profiles, with normal blood pressure, blood sugar, cholesterol levels, and insulin sensitivity. Their health profile might be better than some with lower BMIs.
- “Thin Outside, Fat Inside” (TOFI): Conversely, individuals with a “normal” or even “underweight” BMI can have unhealthy metabolic markers (e.g., high blood sugar, elevated cholesterol, low muscle mass, high visceral fat, and poor overall body composition). Their “normal” BMI can falsely reassure them about underlying health risks.
True health encompasses much more than just a number on the BMI scale. It’s deeply intertwined with your daily choices and overall lifestyle. Our BMI and Lifestyle: Your Guide to Diet, Fitness, and Healthy Habits for a Fitter You emphasizes the foundational role of nutrition, physical activity, sleep, and stress management in achieving genuine well-being, irrespective of your BMI.
BMI Classification vs. Body Composition Realities
| BMI Classification | Example Individual | Typical Body Composition | Health Risk (General) |
|---|---|---|---|
| Overweight/Obese | Bodybuilder/Athlete | High muscle mass, low body fat | Often Low |
| Overweight/Obese | Sedentary Individual | High body fat, low muscle mass | Often High |
| Normal Weight | TOFI (Thin Outside, Fat Inside) Individual | Low muscle, high visceral fat | Potentially High |
| Normal Weight | Healthy Individual | Balanced muscle and fat levels | Low |
“Muscle weighs more than fat. Your BMI won’t tell you the difference, which is why a muscular body might fall into an ‘overweight’ category.”
The Risks of Over-Reliance on BMI (Beyond the Number)

Given the limitations of BMI discussed in the previous section, it becomes clear that relying solely on this single metric carries significant BMI risks for individuals. An overemphasis on BMI can lead to incomplete health assessments, psychological harm, and a narrow view of what true well-being entails. Understanding these BMI disadvantages is crucial for anyone navigating their health journey.
Potential for Misdiagnosis and Misclassification
One of the most profound risks of over-reliance on BMI is the potential for misdiagnosis or misclassification of an individual’s health status:
- False Reassurance: An individual with a “normal” or “healthy” BMI might falsely believe they are in good health, even if their lifestyle is poor or they have underlying metabolic issues (the “TOFI” phenomenon). This false sense of security can lead to delayed medical intervention for rising blood pressure, cholesterol, or blood sugar, simply because a key screening tool provided misleading comfort.
- Unnecessary Concern/Intervention: Conversely, as highlighted by the “Muscular Athlete Paradox,” perfectly healthy, muscular individuals may be incorrectly categorized as “overweight” or “obese.” This can lead to unnecessary concern from healthcare providers, pressure to lose weight (even healthy muscle mass), and potentially unhealthy behaviors or disordered eating patterns in an attempt to fit into a misleading BMI category.
Psychological and Social Impact
The societal emphasis on BMI as a definitive health marker also carries profound psychological and social consequences:
- Weight Stigma and Discrimination: A pervasive risk is the contribution of BMI to weight stigma and discrimination. Individuals in higher BMI categories often face prejudice in healthcare settings, employment, and social interactions. This stigma is not only unjust but can also lead to adverse health outcomes, as it discourages individuals from seeking medical care or adhering to health recommendation.
- Body Image Issues & Disordered Eating: An obsessive focus on achieving or maintaining a “healthy” BMI can fuel negative body image issues, body dissatisfaction, and an unhealthy relationship with food and exercise. For some, this relentless pursuit of a BMI number can be a contributing factor to the development of eating disorders, where the number on the scale overrides actual health. Organizations like the National Eating Disorders Association (NEDA) emphasize the dangers of judging health solely by weight or BMI.
- Hindering Healthcare Engagement: Patients who feel judged or stigmatized by healthcare providers based solely on their BMI might avoid medical appointments, leading to neglected health concerns and delayed preventative care. This avoidance creates a significant barrier to effective healthcare.
Ignoring Other Vital Health Markers: The Holistic View
Perhaps the most critical problem with BMI over-reliance is that it distracts from the comprehensive, multi-factorial nature of health. Focusing solely on a weight-to-height ratio means ignoring other crucial health indicators that paint a far more accurate picture of an individual’s well-being:
- Metabolic Health Markers: This includes regularly monitoring blood pressure, cholesterol levels (LDL, HDL, triglycerides), blood sugar regulation (fasting glucose, HbA1c), and markers of inflammation. These provide direct insight into metabolic function, independent of weight.
- Body Composition & Fat Distribution: Beyond just overall weight, understanding your body fat percentage, muscle mass, and particularly where fat is stored (e.g., dangerous visceral fat around organs vs. subcutaneous fat) offers superior insights into health risks. Measurements like waist circumference are often more indicative of metabolic risk than BMI alone.
- Lifestyle Assessment: A truly holistic approach considers your dietary patterns (quality of food, not just quantity), physical activity levels (regular exercise, not just calorie burning), sleep quality, stress management, and overall emotional well-being. These lifestyle factors are foundational to health.
- Fitness Levels: Your cardiovascular endurance, muscular strength, and flexibility are powerful indicators of health and longevity, often having a stronger correlation with health outcomes than BMI.
- Personal and Family Health History: Genetic predispositions and past medical conditions play a significant role in an individual’s health risk profile, none of which are captured by BMI.
To truly embrace a comprehensive understanding of your health, it’s essential to look beyond the scale. Our BMI and Lifestyle: Your Guide to Diet, Fitness, and Healthy Habits for a Fitter You pillar post delves deeply into how these crucial aspects integrate to form your overall well-being.
“Health is not a single number. Relying too heavily on BMI can lead to misjudgments, stigma, and overlooked health risks.”
Debunking Common BMI Misconceptions: Setting the Record Straight

The widespread use of BMI, combined with a lack of deeper understanding, has unfortunately led to several pervasive BMI misconceptions. These BMI myths can hinder accurate self-assessment, cause unnecessary anxiety, and even delay appropriate medical guidance. It’s time to set the record straight and provide clarity on what BMI truly means – and what it doesn’t.
Misconception 1: “BMI is a diagnostic tool for individual health.”
Debunk: This is perhaps the most fundamental misunderstanding. As discussed, BMI is primarily a screening tool, not a diagnostic one. It’s a quick, inexpensive way to identify individuals who might be at an increased health risk due to their weight-to-height ratio, prompting further investigation. A high BMI doesn’t automatically diagnose obesity or poor health, just as a “normal” BMI doesn’t guarantee good health. A diagnosis requires a comprehensive medical examination by a healthcare professional, considering multiple health indicators.
Misconception 2: “A ‘healthy’ BMI guarantees you’re healthy.”
Debunk: While a BMI within the “healthy weight” range often correlates with lower health risks at a population level, it certainly doesn’t guarantee individual health. The TOFI (Thin Outside, Fat Inside) phenomenon is a perfect example. Individuals can have a seemingly healthy BMI, but possess high levels of visceral fat, low muscle mass, and unhealthy metabolic markers (like elevated blood sugar or cholesterol). These individuals are at risk for metabolic diseases despite their “normal” BMI. This illustrates that health is not merely the absence of a high BMI, but a state of overall well-being encompassing various physiological and lifestyle factors.
Misconception 3: “A high BMI automatically means you’re unhealthy.”
Debunk: This myth contributes heavily to weight stigma and misjudgment. As explored with the “Metabolically Healthy Obese” (MHO) concept, some individuals with a high BMI may have excellent metabolic health, healthy blood markers, and good fitness levels. Their elevated BMI might be due to a high amount of lean muscle mass rather than excess fat. Health is complex and multifactorial; a single high number on the BMI scale should prompt further investigation, not an automatic judgment of ill health. What truly matters is a holistic assessment of body composition, metabolic indicators, and lifestyle habits.
Misconception 4: “BMI applies universally to everyone, regardless of age, gender, or ethnicity.”
Debunk & Empower with Your Tools: This is one of the most significant limitations of BMI and where specialized tools become incredibly valuable. The universal application of standard adult BMI categories overlooks crucial physiological differences across demographics.
- Children & Teens: BMI interpretation for children and adolescents is vastly different from adults. Their bodies are constantly growing and changing, so their BMI is interpreted using age- and sex-specific growth charts and percentiles rather than fixed cutoff points. A “healthy” BMI for a 10-year-old girl, for instance, means her BMI falls between the 5th and 85th percentiles for her age and sex.
- Tool Integration: For accurate and age-appropriate assessments for the younger population, our BMI for Kids Calculator and BMI for Teens Calculator provide interpretations tailored to their unique growth patterns, using official CDC data.
- Seniors: As we age, body composition naturally changes. Muscle mass (sarcopenia) tends to decrease, and body fat might increase or redistribute, even if overall weight remains stable. Furthermore, a slightly higher BMI in older adults might even be protective against certain health risks or provide a reserve during illness. The standard adult BMI categories may not accurately reflect health status or BMI risks in the elderly, and an overly aggressive approach to weight loss in seniors can be detrimental. This highlights another critical limitation of BMI.
- Tool Integration: Recognizing the unique physiological changes of aging, our BMI for Seniors Calculator offers guidance that accounts for these differences, providing more relevant insights for older adults focused on maintaining health and quality of life.
- Men vs. Women: While the general BMI formula is the same, men and women typically have different average body compositions. Women naturally tend to have a higher percentage of body fat than men. While not leading to different BMI categories, understanding these physiological distinctions helps in interpreting the broader health picture.
- Tool Integration: Our BMI for Men Calculator and BMI for Women Calculator help account for typical gender-specific body compositions, offering more personalized insights and ideal weight ranges.
- Ethnic Differences: Research suggests that different ethnic groups may have varying healthy body fat percentages at the same BMI, leading to different health BMI risks profiles. For example, some Asian populations may experience health risks associated with higher body fat at a lower BMI compared to Caucasian populations. This highlights the need for a culturally sensitive and nuanced interpretation of BMI data and is a key limitation of BMI.
BMI Interpretation Across Populations
| Population Group | Key Consideration for BMI Interpretation | How BMI is Interpreted (General) | BMICount Tool |
|---|---|---|---|
| Adults (General) | Used as a population screening tool | Standard fixed BMI categories | General BMI Calculator |
| Children/Teens | Rapid growth and changes in body composition | Age- and sex-specific percentiles | BMI for Kids, BMI for Teens |
| Seniors | Muscle loss and altered body composition with age | Higher BMI may be protective | BMI for Seniors |
| Athletes | High muscle mass can skew results | May be misclassified as “overweight” | BMI for Men, BMI for Women (for ideal weight insight) |
| Ethnic Groups | Differences in body fat distribution at same BMI | May require population-specific thresholds | General awareness or professional consultation |
“BMI interpretation is not ‘one size fits all.’ Your age, gender, and unique body composition matter.”
Beyond BMI: Embracing a Holistic Health Assessment
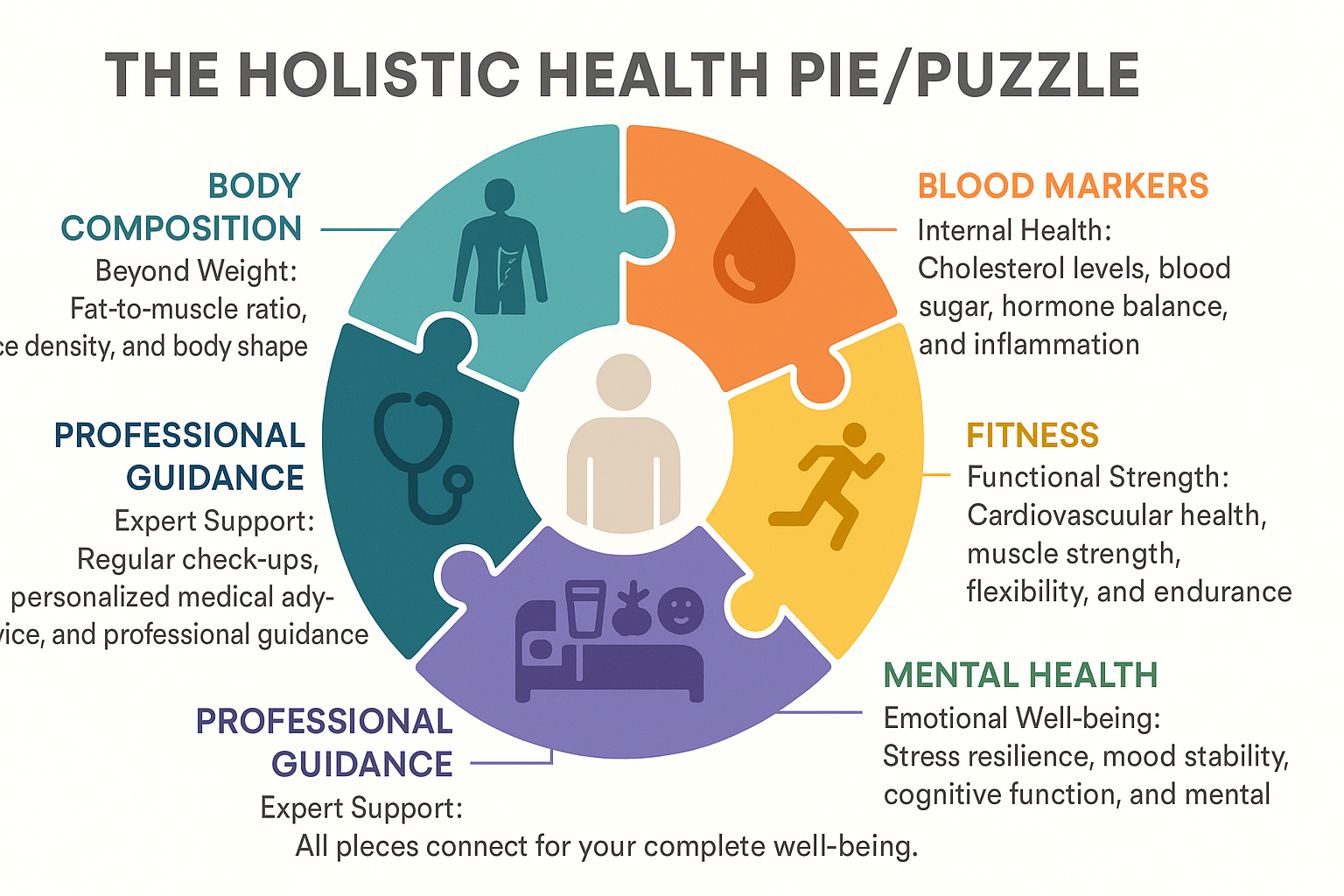
As we’ve thoroughly explored, while BMI serves as a useful initial screening tool, it represents only a small piece of the intricate puzzle that is your overall health. To truly understand your well-being and make informed decisions, it’s essential to look beyond BMI and embrace a comprehensive, holistic health assessment. This multi-dimensional approach considers various physiological indicators, lifestyle factors, and professional guidance, compensating for the inherent limitations of BMI.
Key Complementary Measures for a Complete Picture
A truly insightful health assessment integrates several crucial measures that provide a far more accurate and actionable understanding of your body:
- Waist Circumference & Waist-to-Hip Ratio: These are incredibly important indicators of abdominal fat, particularly the dangerous visceral fat that surrounds internal organs. High levels of visceral fat, regardless of BMI, are strongly linked to increased risks for type 2 diabetes, heart disease, and metabolic syndrome. Measuring your waist circumference provides a direct assessment of this critical risk factor. A general guideline suggests women aim for a waist circumference under 35 inches (88 cm) and men under 40 inches (102 cm).
- Clinical Blood Markers: Your blood work offers a window into your internal metabolic health. Regular checks of the following are crucial:
- Blood Pressure: A key indicator of cardiovascular health.
- Cholesterol Panel: Including LDL (“bad” cholesterol), HDL (“good” cholesterol), and triglycerides, which are vital for assessing heart disease risk.
- Blood Glucose & HbA1c: Essential for evaluating blood sugar regulation and diabetes risk.
- Inflammatory Markers: (e.g., C-reactive protein) can indicate systemic inflammation, linked to various chronic diseases.
- Lifestyle Assessment: Your daily habits profoundly influence your health. A thorough assessment should delve into factors that are crucial beyond BMI:
- Dietary Patterns: Focus on the quality of your diet – emphasizing whole foods, fruits, vegetables, lean proteins, and healthy fats – rather than just calorie counting.
- Physical Activity Levels: Beyond simply exercising, consider your overall daily movement, incorporating varied forms of activity (cardio, strength training, flexibility). Your fitness levels are a powerful predictor of longevity and health.
- Sleep Quality: Adequate, restorative sleep is fundamental for hormonal balance, cognitive function, and metabolic health.
- Stress Management: Chronic stress can negatively impact nearly every bodily system, contributing to weight gain, inflammation, and chronic disease. Effective stress management strategies are vital.
- Emotional Well-being: Mental health significantly impacts physical health. Addressing mood, anxiety, and self-care is part of a complete health picture.
- Fitness Levels: Your actual physical capabilities, not just weight, are a strong predictor of health and longevity. Assessing cardiovascular endurance, muscular strength, and flexibility provides a more direct measure of functional health. A person with a higher BMI who is regularly active and has good cardiovascular fitness may be healthier than a sedentary person with a “normal” BMI.
- Personal Health History & Family History: Your unique medical history and family predispositions to certain conditions (like heart disease, diabetes, or cancer) provide invaluable context for your individual health BMI risks profile. These factors cannot be captured by any single metric, underscoring another limitation of BMI.
The Indispensable Role of Your Healthcare Professional
While understanding these measures is empowering, it’s paramount to remember that interpreting them requires professional expertise. For a truly personalized health assessment, diagnosis, and guidance, always consult a qualified healthcare professional. They can integrate all these factors – your numbers, your lifestyle, your history, and your specific health goals to provide tailored recommendations that empower your journey to optimal well-being, effectively guiding you beyond BMI for your health.
“True health is a symphony of factors: from what you eat and how you move, to your sleep, stress, and every unique marker your body presents.”
Maximize Your Health Insights: Leverage Our Advanced BMI Tools
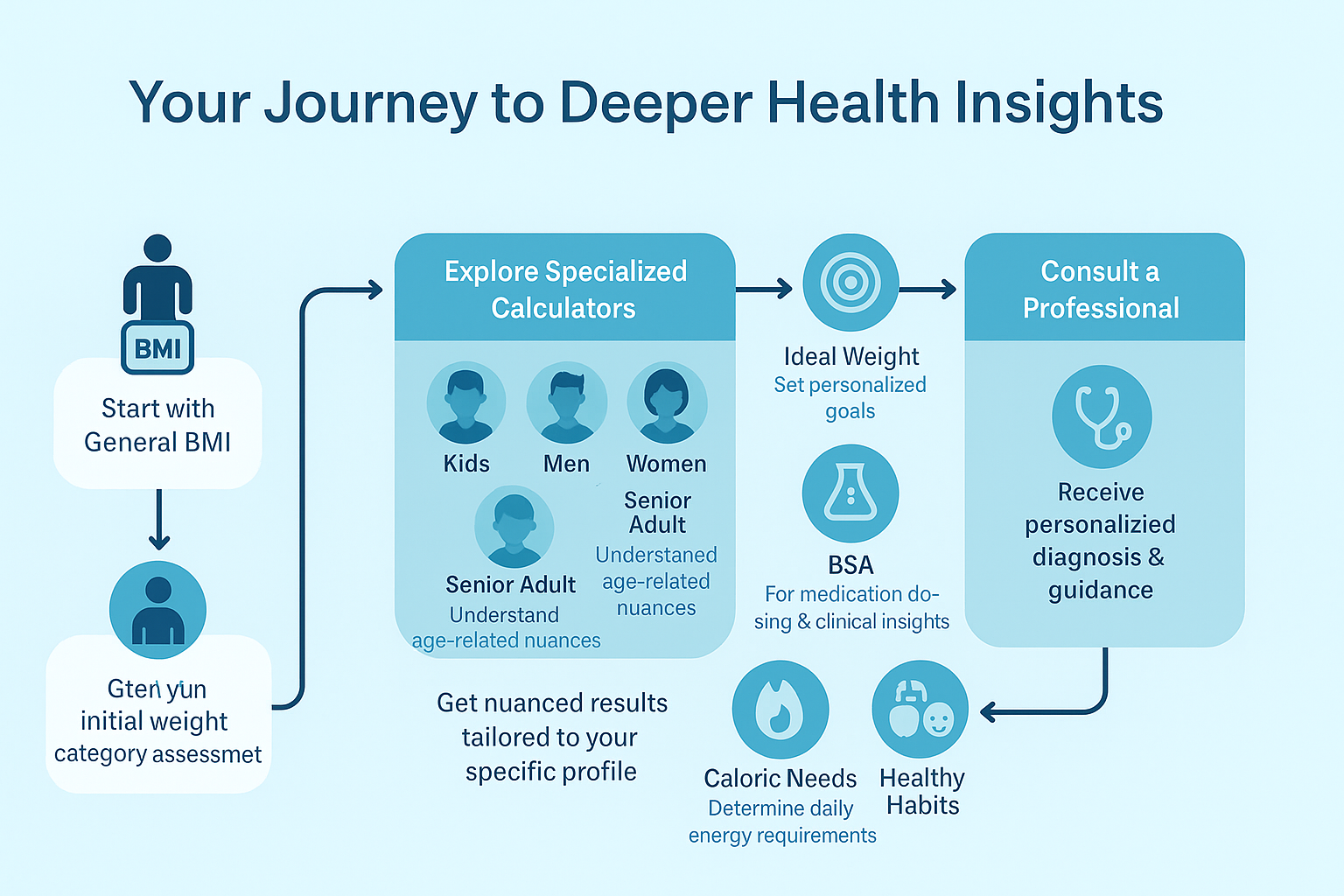
Understanding the nuances of BMI and recognizing the importance of a holistic health assessment are powerful steps on your journey to well-being. At BMI Count, we believe that informed decisions stem from accurate information and accessible resources. That’s why our comprehensive suite of specialized BMI calculators is designed to help you gain a more complete and actionable picture of your health, going beyond BMI’s basic classification and addressing common BMI misconceptions.
Our tools are built to provide more than just a number; they offer personalized health insights that consider various factors often overlooked by generic BMI charts, improving perceived BMI accuracy for individuals. We aim to empower you to interpret your numbers correctly and understand what they truly mean for your body, helping you understand the limitations of BMI.
Here’s how our advanced BMI tools can support your pursuit of a deeper understanding of your health:
- General BMI Calculator: Your Starting Point for Key Metrics
This is where many begin their health journey. Our general calculator provides your BMI classification and initial insights such as your Ideal Weight Range and Body Surface Area (BSA). It’s a quick, accessible way to get a fundamental understanding of your weight-to-height ratio, serving as a reliable starting point for further exploration beyond BMI‘s simple number. - BMI for Men Calculator & BMI for Women Calculator: Tailored Assessments for Gender-Specific Insights
Recognizing that typical body composition differs between men and women (e.g., average body fat percentages and muscle distribution), these specialized calculators provide more nuanced interpretations. They offer a more refined understanding of your BMI in the context of common gender-specific physiological trends, helping you align your health goals with what’s typical for your sex and addressing some limitations of BMI. - BMI for Kids Calculator & BMI for Teens Calculator: Accurate Interpretation for Growing Bodies
For parents and guardians, assessing a child’s weight status requires specific considerations due to ongoing growth and development. Our dedicated calculators for children and teens interpret BMI using official age- and sex-specific growth charts from reputable health organizations. This ensures that their results are accurately understood within the context of their unique developmental stage, providing reliable guidance for healthy growth and improving BMI accuracy for youth. - BMI for Seniors Calculator: Relevant Guidance for Older Adults
As discussed, the aging process brings unique physiological changes, including potential muscle loss (sarcopenia) and shifts in body fat. Our specialized Senior BMI Calculator offers guidance that accounts for these differences, understanding that a slightly higher BMI might sometimes be protective in later life. This tool focuses on promoting health and maintaining quality of life for older adults, moving beyond BMI‘s generic benchmarks and addressing specific limitations of BMI for this age group.
Don’t let a single number define your health or dictate your journey. Use our specialized calculators in conjunction with the knowledge gained from this comprehensive guide to gain a more personalized and empowering understanding of your well-being. These tools are designed to be part of your broader health assessment strategy, providing data points that, when combined with professional medical advice, can truly inform your path to optimal health and mitigate potential BMI risks.
“Our specialized calculators go beyond the basics, offering you the nuanced insights you need to truly understand your body and guide your health journey.”
Frequently Asked Questions
Is BMI a reliable indicator of individual health?
BMI is a useful population-level screening tool, but it’s not a definitive diagnostic tool for individual health. It doesn’t differentiate between muscle and fat, nor does it account for fat distribution, age, gender, or ethnicity.
Why do doctors still use BMI if it has so many limitations?
Doctors use BMI because it’s a simple, inexpensive, and non-invasive screening tool. It helps identify individuals who might need further evaluation for weight-related risks, making it practical for large-scale public health monitoring.
Can a high BMI mean I’m still healthy?
Yes, for some. Highly muscular individuals (like athletes) often have a high BMI due to dense muscle, not excess fat, yet maintain excellent metabolic health. Body composition and metabolic markers are more telling than BMI alone.
Can a “normal” BMI mean I’m unhealthy?
Yes. Individuals with a “normal” BMI can still have high visceral fat and unhealthy metabolic markers (the “Thin Outside, Fat Inside” or TOFI phenomenon). A holistic health assessment is crucial to understand true well-being.
What are better alternatives or complementary measures to BMI for assessing health?
Key measures include body composition analysis (fat vs. muscle), waist circumference, clinical blood markers (blood pressure, cholesterol, blood sugar), and a thorough lifestyle assessment (diet, activity, sleep, stress).
How does BMI interpretation differ for specific groups like children or seniors?
For children and teens, BMI uses age- and sex-specific growth charts. For seniors, a slightly higher BMI can sometimes be protective due to age-related body changes. Our specialized BMI for Kids Calculator, BMI for Teens Calculator, and BMI for Seniors Calculator offer accurate interpretations.
Does ethnicity impact how BMI should be interpreted?
Yes. Research shows that different ethnic groups may have varying body fat percentages at the same BMI, leading to different health risk thresholds. This highlights a limitation of BMI and the need for nuanced interpretation.
Should I try to achieve a “normal” BMI at all costs?
No. Obsessing over a specific BMI can lead to unhealthy behaviors and body image issues. Focus instead on sustainable lifestyle habits, healthy body composition, and positive metabolic markers for overall well-being. Consult a healthcare professional for personalized goals.
Conclusion: Empowering Your Health Journey with Informed Decisions
We’ve embarked on a detailed exploration, moving beyond BMI to unveil the full story of your health. What began as a simple number has revealed itself to be a complex, multifaceted indicator with significant strengths as a population-level screening tool, but equally important limitations of BMI when applied to individual health. We’ve meticulously debunked common BMI misconceptions, addressed the potential BMI risks of over-reliance, and charted a path towards a truly holistic health assessment.
The core message is clear: BMI accuracy is limited for individual assessment; it is a helpful starting point, a piece of the puzzle, but never the entire picture. Your health is a dynamic interplay of factors including your unique body composition, vital blood markers, consistent lifestyle habits, fitness levels, and mental well-being. It’s a journey, not a static destination defined by a single metric.
We encourage you to take control of your health narrative by looking beyond BMI‘s simplistic classifications. Focus on sustainable lifestyle habits that truly nourish your body and mind, engage in consistent physical activity, prioritize quality sleep, and manage stress effectively. Most importantly, always consult with a qualified healthcare professional. They are your most valuable resource, capable of integrating all these elements into a personalized plan tailored to your specific needs and goals, helping you avoid potential BMI risks and BMI misconceptions.
At BMI Count, we are dedicated to providing you with accurate, evidence-based information and practical tools to empower you on your personal health journey. Our specialized BMI calculators are here to offer you more nuanced insights, helping you understand your body better. Use these resources wisely, engage with your healthcare provider, and embrace a comprehensive view of your well-being. Understand your body, make informed choices, and thrive.




