In the vast landscape of health and wellness, few metrics are as widely cited, debated, and often misunderstood as the Body Mass Index, or BMI. From routine doctor’s visits to global health reports, the acronym BMI has become a ubiquitous shorthand for assessing an individual’s weight relative to their height.
Yet, for many, the BMI calculation remains a nebulous concept. Its origins are often shrouded in history, and its implications subject to broad interpretation. Is it a definitive measure of health, or merely a starting point for a deeper conversation?
This comprehensive guide aims to pull back the curtain on this foundational health metric. We will embark on a scientific journey, meticulously exploring the BMI formula at its core. We’ll trace the fascinating history of Body Mass Index research, and delve into the complexities of how BMI data is collected, analyzed, and applied on both individual and population levels.
Crucially, we will also critically examine the well-documented limitations of BMI. This offers a balanced perspective that acknowledges its utility while highlighting its nuances.
At BMI Count, our commitment is to precision and clarity. We believe that understanding the scientific underpinnings of health assessments is paramount. Our tools provide accurate BMI calculations derived from the most trusted global health organizations, including the World Health Organization (WHO), the National Institutes of Health (NIH), and the Centers for Disease Control and Prevention (CDC), ensuring you receive reliable insights. For a quick and accurate assessment, explore our General BMI Calculator.
“BMI is more than just a number; it’s a gateway to understanding population health trends and individual well-being.”
The Foundational Blueprint: Deconstructing the BMI Formula and Calculation
To truly grasp the implications and utility of the Body Mass Index, one must first understand its bedrock: the BMI formula and the underlying principles of its BMI calculation. While seemingly straightforward, this simple equation is the cornerstone of a global health metric. It offers a quick and accessible snapshot of weight status. Understanding its origins and mechanics is essential for interpreting its output accurately and appreciating its scientific significance.
The Genesis of BMI: Adolphe Quetelet and His Legacy
The journey of the BMI begins not in a medical clinic, but in the mind of a 19th-century Belgian mathematician and astronomer, Adolphe Quetelet. In the 1830s, Quetelet developed what he called the “Quetelet Index.” This was part of his groundbreaking studies on “social physics,” aiming to describe the characteristics of the “average man.”
His index, which related weight to the square of height, was designed purely as a statistical tool for population-level observations. It was not intended as a diagnostic measure for individual health. It wasn’t until 1972 that American physiologist Ancel Keys coined the term “Body Mass Index” and championed its use in epidemiological studies. He recognized its value as a simple, reliable indicator for comparing weight status across diverse populations.
This historical context is vital. The BMI calculation was initially a statistical instrument, and its current widespread clinical application represents an evolution of its original intent.
Decoding the Standard BMI Formula: Metric vs. Imperial
At its heart, the BMI formula is elegantly simple, providing a ratio of a person’s weight to their height. This standardization allows for comparisons across different individuals and groups, regardless of their absolute size. The formula varies slightly depending on whether you are using the metric or imperial system of measurement.
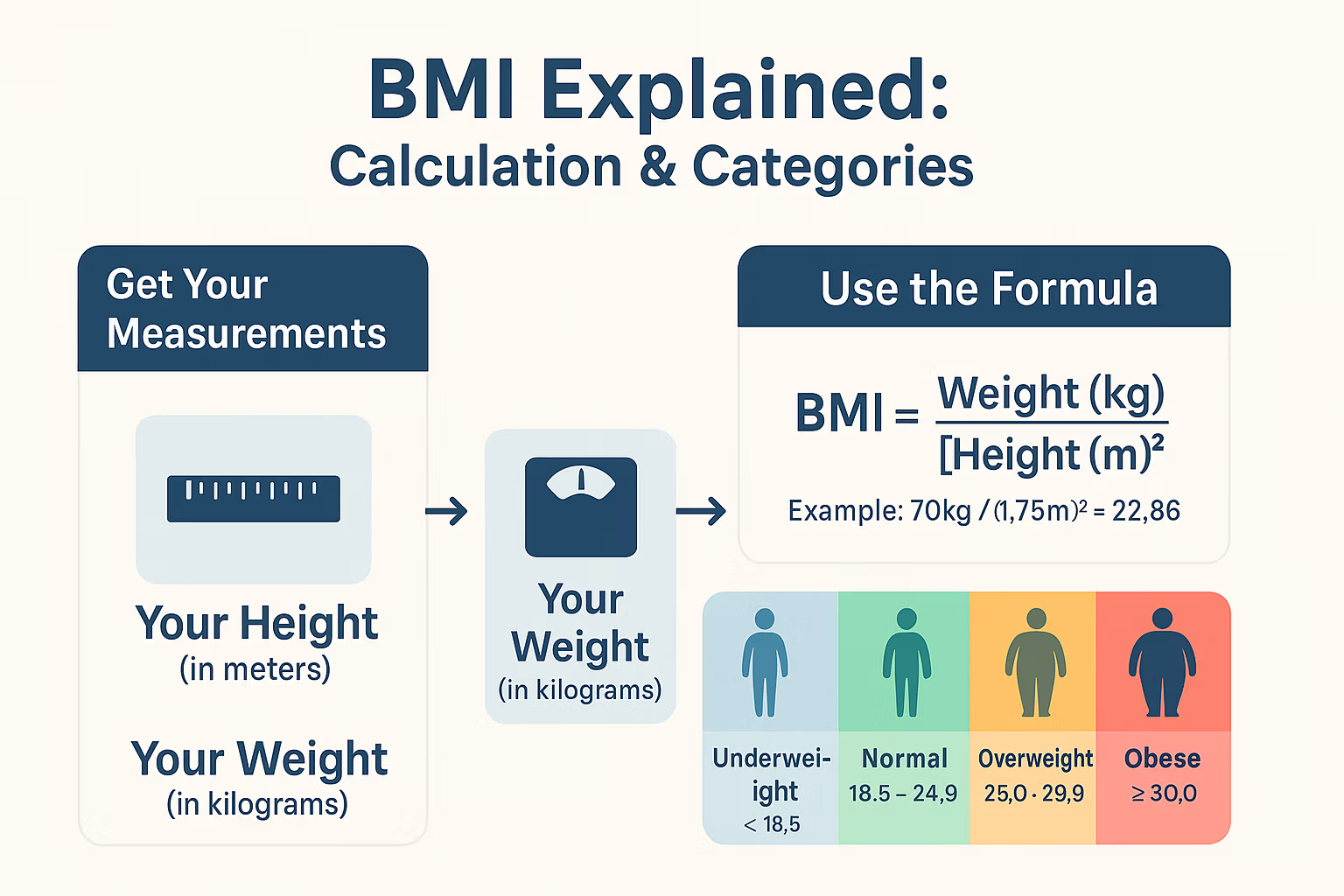
Metric System: The most commonly used version globally, particularly in scientific and medical contexts, is: BMI=mass(kg)/height(m)2 Here, ‘mass’ is measured in kilograms (kg), and ‘height’ is measured in meters (m). The height is squared to normalize the value, accounting for the non-linear relationship between weight and height in body shape.
Imperial System: For those using pounds and inches, the formula includes a conversion factor: $BMI = (mass(lbs) \* 703) / height(in)^2$ In this formula, ‘mass’ is in pounds (lbs), ‘height’ is in inches (in), and 703 is the conversion factor to align the units.
This fundamental BMI calculation forms the basis for assessments worldwide.
BMI Formula Breakdown (Metric & Imperial)
| Unit System | Formula | Explanation of Variables |
|---|---|---|
| Metric | BMI=fractextMass(kg)textHeight(m)2 | Mass in kilograms, Height in meters (squared) |
| Imperial | BMI=fractextMass(lbs)times703textHeight(in)2 | Mass in pounds, Height in inches (squared), 703 is a conversion factor |
The Categorization System: Understanding BMI Ranges
Once the BMI calculation is complete, the resulting number is then placed into standard categories. These categories indicate an individual’s weight status relative to population norms. They are globally recognized and are fundamental to the interpretation of BMI in clinical and public health settings.
The most widely accepted categories, established by organizations like the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC), are:
- Underweight: BMI less than 18.5
- Normal Weight (or Healthy Weight): BMI between 18.5 and 24.9
- Overweight: BMI between 25.0 and 29.9
- Obesity Class I: BMI between 30.0 and 34.9
- Obesity Class II: BMI between 35.0 and 39.9
- Obesity Class III (or Severe/Morbid Obesity): BMI 40.0 or greater
These ranges are critical for guiding health conversations. They help identify potential health risks and inform public health strategies. It’s important to remember that while these categories provide a standardized framework, individual assessments should always consider other health factors.
For a personalized BMI calculation and an understanding of where you fall within these ranges, you can use our specialized calculators:
Beyond the Basic Number: Advanced Calculations and Interpretations
While the core BMI formula provides a simple weight-to-height ratio, the science of anthropometry and health assessment has evolved to offer more granular insights. Advanced calculations, often integrated into sophisticated tools like those at BMI Count, delve deeper than the single BMI number.
Concepts such as Body Surface Area (BSA), calculated using formulas like Mosteller or Du Bois, become crucial in specific medical contexts. For example, they are used in determining drug dosages or assessing burn areas. Similarly, the concept of an “ideal weight range” is often derived from statistical analyses of healthy populations. It takes into account age and sex, providing a more tailored target than a simple BMI category.
These advanced interpretations demonstrate that while the fundamental BMI calculation is simple, its application in health science is far more nuanced and dynamic. This provides a more complete picture of an individual’s health landscape.
“The simplicity of the BMI formula belies its profound impact on public health understanding.”
Unpacking the Data: How BMI Information is Collected, Analyzed, and Utilized
Beyond the individual BMI calculation, lies a fascinating and crucial realm: the collection, analysis, and utilization of BMI data on a broader scale. This aggregate information transforms a simple individual metric into a powerful epidemiological tool. It enables researchers and public health officials to identify trends, assess population health, and design effective interventions. Understanding how this data is gathered and interpreted is key to appreciating its role in shaping health policy and informing global wellness strategies.
Sources of BMI Data: National Health Surveys and Clinical Records
Robust insights from BMI data are built upon extensive and systematic collection efforts. The primary sources for this invaluable information typically fall into two main categories: large-scale national health surveys and aggregated clinical records.
National health surveys, like the National Health and Nutrition Examination Survey (NHANES) in the United States, are cornerstone initiatives. Similar large-scale demographic and health surveys are conducted by national agencies in India and across the globe. These surveys collect health and nutrition information from representative population samples.
They involve interviews, physical examinations (including height and weight measurements for BMI calculation), and laboratory tests. Their rigorous methodologies ensure that collected BMI data accurately reflects the weight status of the wider population. This includes diverse age groups, genders, and socioeconomic strata. Consistent collection over decades also allows for tracking trends in obesity and underweight prevalence.
Complementary to these surveys, aggregated clinical records contribute significantly. Data from hospitals, clinics, and electronic health systems, when anonymized and compiled, offer real-world insights. They reveal health patterns within specific regions or patient cohorts. This type of BMI data analysis can highlight the prevalence of certain conditions linked to BMI within clinical populations and inform healthcare resource planning. The synergy between these diverse sources creates a comprehensive picture of public health challenges.
Statistical Approaches to BMI Data Analysis
Raw numbers of BMI data only gain meaning through sophisticated statistical analysis. Epidemiological studies, which examine health patterns and causes in populations, rely heavily on these techniques. Researchers use both cross-sectional studies (snapshots at a single point in time) and longitudinal studies (tracking individuals over extended periods).
Through BMI data analysis, statisticians identify correlations between BMI and various health outcomes. These include the risk of developing type 2 diabetes, cardiovascular diseases, or certain cancers. They employ metrics like prevalence (proportion with a condition) and incidence (rate of new cases) to quantify health burdens.
Advanced statistical models help control for confounding variables. This allows for a clearer understanding of observed associations within BMI data. This rigorous approach transforms raw figures into actionable insights. It helps pinpoint risk factors and potential areas for public health intervention.
Key Statistical Metrics Used in BMI Data Analysis
| Metric | Brief Explanation | Relevance to BMI Data |
|---|---|---|
| Prevalence | Proportion of individuals in a population with a condition at a specific time. | Shows the overall burden of underweight, overweight, or obesity in a population. |
| Incidence | Rate at which new cases of a condition occur over a period. | Indicates how quickly new cases of overweight/obesity are developing, revealing trends. |
| Correlation | Statistical measure of how two variables move in relation to each other. | Identifies relationships between BMI and other health markers (e.g., blood pressure, cholesterol). |
| Regression Analysis | Statistical process for estimating the relationships among variables. | Predicts health outcomes based on BMI and other factors, assessing impact. |
Interpreting BMI Data: Population Trends vs. Individual Health Assessments
A crucial distinction in the world of BMI is its interpretation at different scales. While your BMI calculation provides a snapshot of your individual weight status, the true power of BMI data often lies in its application to population trends. For public health professionals, aggregated BMI data helps identify overall shifts in national or regional health.
For instance, a rising average BMI or an increasing prevalence of obesity within a specific demographic can signal a widespread public health concern. This prompts targeted interventions.
However, it’s vital not to conflate population trends with individual health assessments. A single BMI value, particularly at the individual level, offers limited insight into overall health. An individual might fall into an “overweight” BMI category. Yet, they could possess high muscle mass, be metabolically healthy, and engage in regular physical activity.
Conversely, someone in the “normal” BMI range could have high visceral fat, a sedentary lifestyle, and underlying metabolic issues. This highlights the importance of using BMI data for population monitoring and screening. It should never be the sole determinant of an individual’s health. For a more comprehensive discussion on BMI’s accuracy and common misconceptions, read our article: Unveiling BMI: Accuracy, Risks, and Misconceptions.
The Role of BMI Data in Public Health Policy and Interventions
Insights from BMI data analysis are instrumental in shaping public health policy and developing effective interventions. Governments and health organizations worldwide rely on this information.
First, to allocate resources. Understanding where the burden of weight-related issues is highest helps direct funding towards prevention programs, healthcare services, and research.
Second, to design campaigns. BMI data informs the creation of targeted public awareness campaigns about healthy eating, physical activity, and weight management. These are tailored to specific demographics or regions most affected.
Third, to monitor progress. By consistently collecting BMI data, health agencies can track the effectiveness of ongoing programs and policies, making adjustments as needed. For example, if BMI data shows a persistent rise in childhood obesity, it can lead to policy changes regarding school nutrition or physical education.
Finally, to identify risk factors. Large-scale BMI data helps pinpoint environmental or societal factors contributing to unhealthy weight trends. This guides broader policy changes, such as urban planning that encourages walking and cycling, or regulations on food marketing.
These data-driven decisions are critical for fostering healthier communities. They help address the complex challenges posed by evolving weight trends globally.
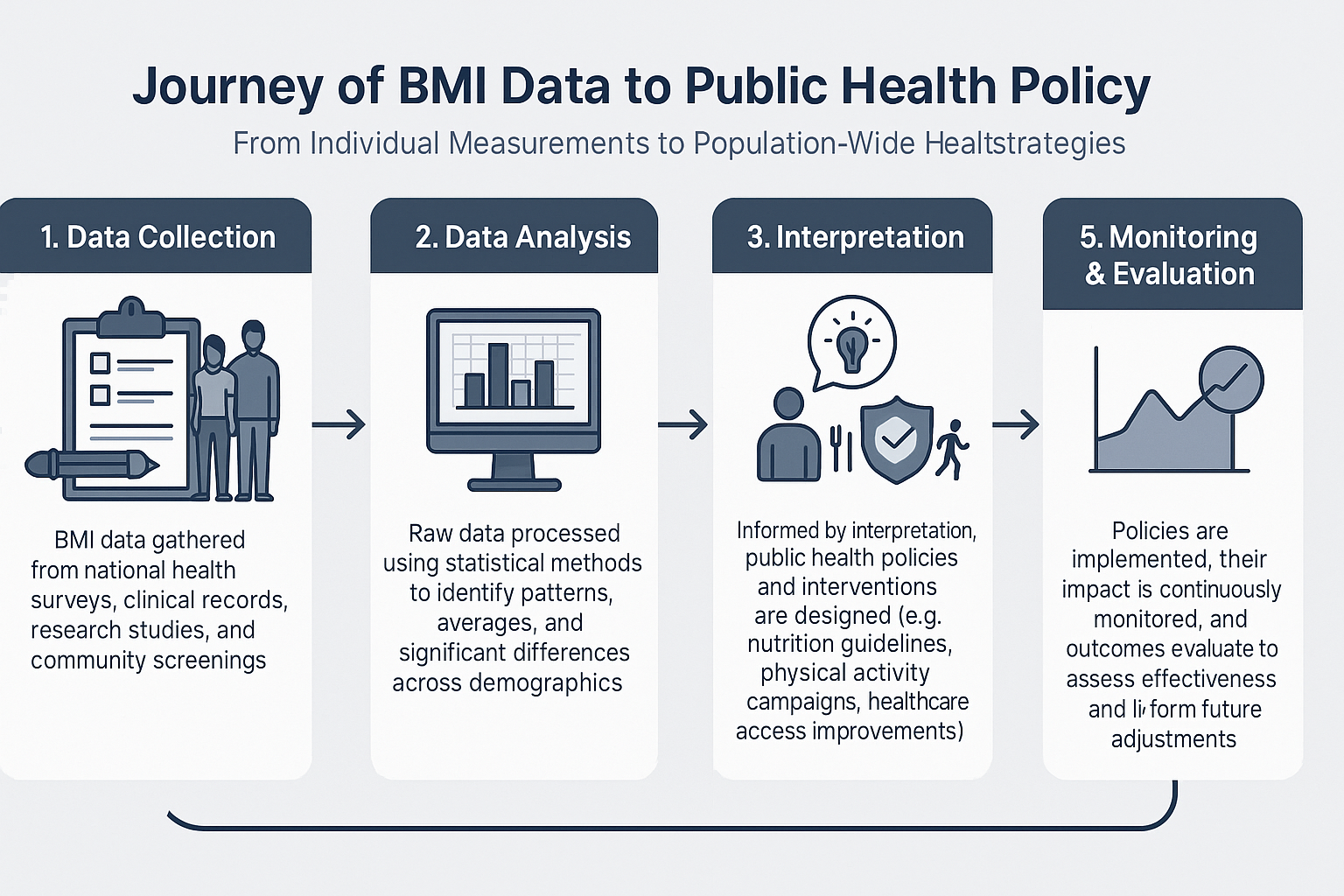
“Aggregate BMI data reveals societal health patterns, guiding critical public health interventions.”
The Scientific Pursuit: Decades of Body Mass Index Research
The Body Mass Index, while a seemingly simple measure, has been the subject of relentless scientific scrutiny and extensive Body Mass Index research for decades. This continuous inquiry aims to refine its utility, understand its associations with various health outcomes, and explore the intricate factors that influence body weight. Far from static, the body of BMI research is constantly evolving, shedding light on the complex interplay between biology, environment, and lifestyle.
Milestones in Body Mass Index Research: From Correlation to Causation
The history of Body Mass Index research is marked by significant milestones. It transitioned from initial observations of correlation to more rigorous attempts at establishing causation. Early studies, particularly those in the mid-20th century, began to identify patterns between higher BMI values and increased risks for certain chronic diseases. This foundational work sparked widespread interest in using BMI as a public health screening tool.
Subsequent BMI research leveraged large cohort studies. These studies tracked populations over long periods, strengthening the evidence for BMI’s predictive power regarding health outcomes. Methodological advancements allowed researchers to control for confounding variables. This helped in isolating the independent effects of BMI, deepening our understanding of its role in health.
BMI’s Association with Health Outcomes: A Review of Key Research Findings
A significant portion of Body Mass Index research has focused on establishing the clear links between BMI and a spectrum of health outcomes. Extensive studies consistently demonstrate a strong association between higher BMI categories (overweight and obesity) and an increased risk of developing numerous non-communicable diseases.
These include Type 2 Diabetes, cardiovascular diseases (such as heart attack and stroke), certain types of cancer (e.g., colorectal, breast, kidney), hypertension, dyslipidemia, osteoarthritis, and sleep apnea. BMI research has often shown a “dose-response” relationship. This means that as BMI increases beyond the healthy range, the risk of these health conditions tends to rise proportionally.
Conversely, research also examines the health implications of being in the underweight category. This can be associated with compromised immune function, osteoporosis, and other nutritional deficiencies. This vast body of evidence underscores BMI’s value as a broad health indicator.
Genetic, Environmental, and Lifestyle Factors in BMI Research
Contemporary Body Mass Index research acknowledges that BMI is not solely a reflection of individual choices. It’s a complex phenotype influenced by a dynamic interplay of genetic, environmental, and lifestyle factors. Genetic studies, including twin and family studies, have revealed a significant heritable component to BMI, suggesting that our genes can predispose us to certain weight ranges. However, genetics alone do not explain the rapid rise in obesity prevalence seen globally.
Environmental factors play a crucial role. This includes access to nutritious food, the built environment (e.g., walkability of neighborhoods), and exposure to obesogenic factors. Lifestyle elements, such as dietary patterns, physical activity levels, sleep quality, and stress management, are also extensively studied in BMI research. Understanding these multifaceted influences is critical for developing effective, holistic strategies to promote healthy weight. For more insights on the practical aspects of managing these factors, delve into our comprehensive guide: BMI and Lifestyle: Your Guide to Diet, Fitness, and Healthy Habits for a Fitter You.
Emerging Frontiers in BMI Science
The field of Body Mass Index research is continuously evolving, pushing the boundaries of our understanding. Current research is exploring more nuanced categories, such as “metabolically healthy obesity,” where individuals with an elevated BMI may not exhibit metabolic abnormalities, challenging traditional assumptions. Personalized nutrition, leveraging genetic and microbiome data, is another burgeoning area. This research aims to understand how individual biological responses to food might influence BMI and overall health.
Scientists are also investigating new body composition metrics that go beyond BMI. These include visceral fat measurements and advanced imaging techniques. These efforts are part of a broader push to find more precise indicators of health risk than weight-to-height ratio alone. This ongoing scientific pursuit ensures that our comprehension of body mass and health remains dynamic and evidence-based.

“Rigorous Body Mass Index research continually refines our understanding, moving beyond simple correlations to complex interactions.”
A Balanced Perspective: Navigating the Limitations and Nuances of BMI
While the Body Mass Index remains a widely used and valuable screening tool in health and epidemiology, a truly comprehensive understanding of its science necessitates acknowledging its inherent limitations of BMI. No single metric can perfectly capture the complexity of human health. Relying solely on BMI can lead to misinterpretations and potentially inaccurate health assessments. It is a tool, not a definitive diagnosis, and its utility is maximized when understood within its proper context.
The Body Composition Conundrum: Why Muscle Matters More Than Mass
One of the primary limitations of BMI is its inability to differentiate between fat mass and lean muscle mass. The BMI calculation uses only total body weight and height. It cannot distinguish if that weight comes from muscle, bone, water, or fat.
This fundamental flaw means that individuals with a high amount of muscle, such as athletes, bodybuilders, or very active individuals, may have a high BMI. They could even fall into the “overweight” or “obese” categories, despite having very low body fat percentages and excellent metabolic health.
Conversely, some individuals may have a “healthy” or “normal” BMI, but still carry a disproportionately high amount of body fat. This condition, often termed “normal weight obesity” or “TOFI” (Thin Outside, Fat Inside), carries similar health risks to overt obesity. For a deeper dive into the accuracy of BMI and common misconceptions, explore our detailed article: Unveiling BMI: Accuracy, Risks, and Misconceptions.
Demographic Variances: BMI Across Age, Gender, and Ethnicity
Another significant nuance in the interpretation of BMI lies in its application across different demographic groups. The standard BMI categories (Underweight, Normal, Overweight, Obese) were primarily developed based on data from Caucasian adult populations. This introduces limitations of BMI when applied universally.
For children and teenagers, BMI is interpreted differently, using age- and sex-specific growth charts rather than fixed thresholds. This accounts for rapid changes in body composition during growth spurts. Similarly, for senior adults (60+), a slightly higher BMI might be considered protective against certain health issues. This is due to age-related muscle loss and changes in bone density.
Furthermore, Body Mass Index research indicates that optimal BMI ranges can vary across different ethnic groups. For instance, some Asian populations may experience increased health risks at lower BMI values compared to Caucasian populations. This highlights the importance of context. You can explore our specialized calculators for these specific groups, which account for these unique considerations:
BMI and Athletes: An Important Exception
The case of athletes often serves as the most prominent example of the limitations of BMI. Professional athletes, particularly those in sports requiring significant muscle mass (e.g., American football players, rugby players, weightlifters), frequently have BMIs well above the “overweight” or “obese” thresholds. Their high muscle density, which is heavier than fat, skews the BMI calculation upwards. This classification is clearly inaccurate for assessing their health risks, as their body composition is dominated by lean mass, not excess fat. For these individuals, BMI is simply not an appropriate standalone health indicator.
Beyond the Number: Complementary Measures for Comprehensive Health Assessment
Given the inherent limitations of BMI, health professionals advocate for its use as a screening tool in conjunction with other health assessments. A holistic understanding of health requires considering a range of complementary measures that provide a more complete picture of body composition and risk.
These include:
- Waist Circumference: Measures abdominal fat, which is metabolically more active and linked to higher disease risk.
- Waist-to-Hip Ratio: Another indicator of central obesity and fat distribution.
- Body Fat Percentage: Directly measures the proportion of fat in the body. This is a more accurate indicator of adiposity than BMI. This can be assessed through various methods like skinfold measurements, bioelectrical impedance analysis (BIA), or DEXA scans (Dual-energy X-ray absorptiometry).
- Blood Pressure, Cholesterol Levels, and Blood Glucose: Crucial indicators of metabolic health that should always be considered alongside BMI.
- Lifestyle Factors: Diet, physical activity levels, sleep quality, and stress management provide invaluable context.
These additional metrics, combined with a clinician’s judgment, offer a far more comprehensive and personalized health assessment than BMI alone.

“Understanding the limitations of BMI is as crucial as understanding its calculation; it’s a tool, not the entire picture of health.”
Bridging Science and Application: How Advanced BMI Tools Leverage Data
The vast body of Body Mass Index research and BMI data we’ve discussed forms the bedrock for modern health assessment tools. While understanding the core BMI formula and its limitations of BMI is crucial, the true power emerges when these scientific principles are applied to provide actionable, personalized insights. Leading health platforms like BMI Count exemplify this integration. They transform complex scientific data into user-friendly tools that empower individuals with a deeper understanding of their health status. These tools go far beyond a simple BMI calculation. They leverage intricate algorithms and established scientific models to offer a more comprehensive health snapshot.
The Power of Personalized Data: BMI Count’s Advanced Insights
At BMI Count, we are dedicated to providing a precise and scientifically-backed assessment. Our tools don’t just give you a single BMI number. Instead, they utilize the scientific principles, BMI data analysis, and advanced formulas derived from trusted sources like WHO, NIH, and CDC to deliver a suite of detailed outputs. These insights are designed to offer a more holistic view of your health.
Consider the following advanced metrics and their scientific basis:
- Ideal Weight Range: This isn’t a random guess. It’s often derived from extensive BMI data of healthy populations and takes into account factors like age, gender, and sometimes even ethnicity. This range represents a statistically healthy weight corridor associated with the lowest risk of certain chronic diseases.
- Body Surface Area (BSA – Mosteller, Du Bois): BSA is a more complex physiological calculation derived from height and weight. It’s scientifically critical in various medical fields for precise measurements. For instance, BSA is used to accurately determine drug dosages (especially chemotherapy), fluid requirements in burn victims, and even the calculation of cardiac output. Its inclusion reflects a deeper application of anthropometric science.
- Caloric Needs (Maintain/Goal): These estimations are grounded in the science of metabolic rate and energy balance. Formulas like the Mifflin-St Jeor equation (or similar, depending on the tool’s sophistication) use your age, gender, height, weight, and activity level to estimate your Basal Metabolic Rate (BMR) and Total Daily Energy Expenditure (TDEE). This scientific foundation allows us to provide targeted caloric guidance for weight maintenance or achieving a specific goal.
- Activity Insights & Healthy Habit Focus: Beyond numbers, our tools translate scientific understanding into practical lifestyle advice. Based on your BMI calculation and health goals, these insights are tailored to guide users towards beneficial physical activity levels and healthy eating habits. They reflect current Body Mass Index research on lifestyle interventions for weight management and overall well-being.
BMI Count’s Advanced Result Metrics and Their Scientific Basis
| Metric | Brief Explanation | Scientific Relevance |
|---|---|---|
| Ideal Weight Range | A calculated weight bracket statistically associated with the lowest health risks for your demographic. | Based on population BMI data and epidemiological studies linking ranges to health outcomes. |
| Body Surface Area (BSA) | A calculated measure of the total surface area of the human body. Utilizes formulas like Mosteller or Du Bois. | Crucial for precise medical calculations, including drug dosages (e.g., chemotherapy), fluid administration for burns, and cardiac index. |
| Caloric Needs | Estimates the daily energy (kcal) required to maintain current weight or reach a target weight. | Derived from metabolic rate formulas (e.g., Mifflin-St Jeor), accounting for Basal Metabolic Rate (BMR) and Total Daily Energy Expenditure (TDEE) based on activity levels. |
| Activity Insights | Personalized suggestions for physical activity based on your BMI and health status. | Aligned with public health guidelines and Body Mass Index research on the role of exercise in weight management and chronic disease prevention. |
| Healthy Habit Focus | Tailored advice on nutrition, sleep, hydration, and other lifestyle factors. | Integrates findings from Body Mass Index research and general health science on the impact of holistic lifestyle on long-term well-being and weight maintenance. |
Tailoring Insights: Specific Considerations for Different Demographics
Recognizing that a single BMI calculation doesn’t apply equally to all, advanced tools like BMI Count provide specialized calculators for diverse demographics. This reflects the scientific understanding that different age groups and genders have unique physiological characteristics and growth patterns.
- Kids and Teens: Their BMI is interpreted using age- and sex-specific growth charts, acknowledging their ongoing development. These charts are derived from extensive BMI data collected over decades by organizations like the CDC. You can find specialized tools for BMI Calculator for Kids 2-12 and BMI Calculator for Teens 13-17.
- Men and Women: While the core BMI formula is the same, interpreting “ideal weight ranges” or caloric needs often considers gender-specific metabolic differences and body composition norms. Explore our dedicated calculators for BMI Calculator for Men and BMI Calculator for Women.
- Senior Adults: For individuals 60+, Body Mass Index research indicates that slightly higher BMIs might be associated with better health outcomes. Our BMI Calculator for Senior Adults 60+ provides tailored interpretations that account for age-related changes in body composition and metabolism.
At BMI Count, our dedication to accuracy ensures that these nuanced BMI calculations are grounded in the latest scientific consensus and guidelines from trusted platforms, offering truly relevant insights. For a broader perspective on all aspects of BMI, consult our Your Complete Guide to Understanding BMI.
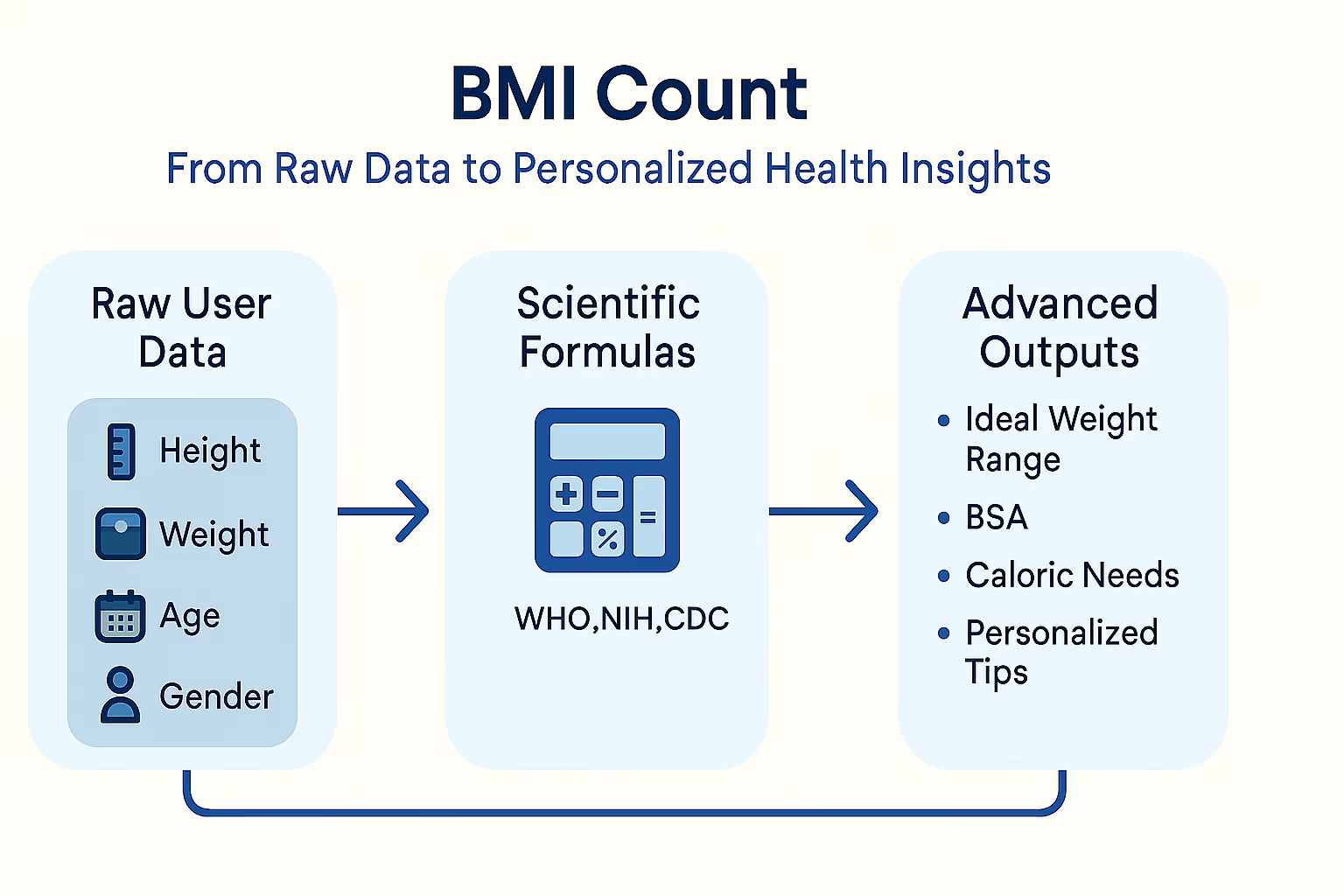
“At BMI Count, we transform complex BMI science and data into clear, actionable insights for your personalized health journey.”
Conclusion
Our journey through the “Science and Data Behind BMI Calculations” has unveiled the intricate layers of this widely used health metric. We’ve deconstructed the fundamental BMI formula, explored the extensive world of BMI data collection and analysis, and delved into decades of insightful Body Mass Index research. Crucially, we’ve also candidly examined the inherent limitations of BMI, understanding that it’s a valuable screening tool when viewed in a balanced context.
A thorough understanding of BMI empowers both individuals and public health initiatives. It allows for more informed health decisions and more effective population-level strategies. At BMI Count, our dedication to accuracy ensures our tools transform complex scientific principles into clear, actionable insights for your personalized health journey.
We invite you to explore our free, scientifically-backed calculators to gain a more precise understanding of your own health metrics. Empower yourself with accurate data.




